Assessing The Efficacy of Semaglutide on Glycaemia Control and Weight Reduction among Patients with Type 2 Diabetes at the Outpatient Department of Teaching Hospital
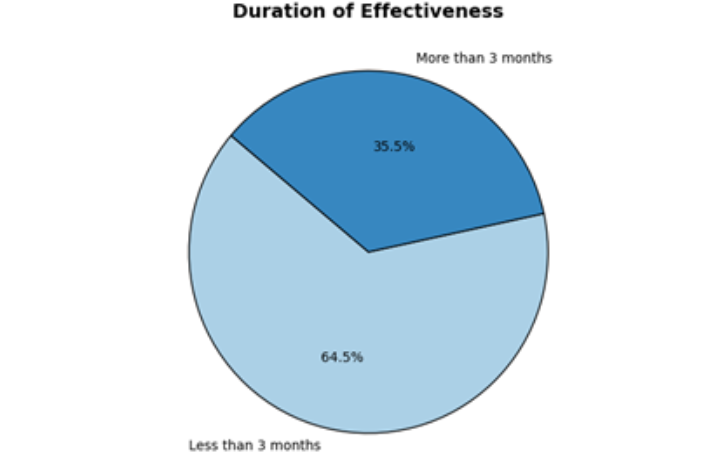
Figure 1: Pie Chart of the Study Population Based on the Effectiveness of Medication In recent research conducted on 31 Type 2 diabetes patients, valuable insights were gathered into both the demographics of the study population and their experiences with diabetes management. The study aimed to highlight factors such as gender, age, medication effectiveness, side effects, and knowledge regarding diabetes treatment. Here, we break down the key findings of this study. Demographics of the Study Population The study revealed a predominantly female population, with 93.5% of participants being women. The age distribution showed that the majority (64.5%) were between 18-39 years old. When it came to education, a significant 64.5% of participants had attained a bachelor’s degree or higher, indicating a highly educated group. In terms of employment, the majority (48.4%) were fully employed, while 45.2% were retired. Notably, a large portion (87.1%) of the population had a monthly income above 50,000 BDT, though only 6.5% had health insurance coverage, highlighting a gap in access to healthcare services for many participants. In terms of diabetes history, 38.7% of the participants had been diagnosed with Type 2 diabetes within the past year, while another 38.7% had been living with the condition for 1-5 years. The majority (77.4%) were taking medications for their diabetes, with the most common being Comet XR (12.6%), Metformin (6.3%), and Diamicron (5.0%). Notably, 83.9% of the participants had reported recent changes in their diabetes condition. A concerning 54.8% of participants also had comorbidities, with high blood pressure being the most common (35.4%). Semaglutide, a medication used for managing diabetes, was regularly used by 93.5% of the participants, though 64.5% experienced side effects. The primary challenge in using Semaglutide was its cost (67.7%), but many patients reported positive outcomes, with 83.9% experiencing weight loss. Medication Effectiveness and Side Effects and Weight Loss After Semaglutide Use When examining the effectiveness of diabetes treatments, the study found that 64.5% of participants reported the effectiveness of their medication lasted less than three months. Additionally, the bar chart revealed that most patients (75%) had a modest reduction of 1-2% in symptoms, while a smaller percentage (7.1%) experienced a 2-3% reduction. Semaglutide’s side effects were another significant finding of the study. A considerable number of participants experienced nausea (25 patients), vomiting (20 patients), dizziness (14 patients), and even stomach pain or drowsiness (2 patients). Despite the side effects, Semaglutide led to significant weight loss in many participants, with the majority (83.9%) losing weight after regular use. The most common weight loss category was between 3.5-7 kg, observed in over 10 individuals. Knowledge About Diabetes The study population exhibited a high level of diabetes-related knowledge. An overwhelming 93.5% of participants recognized that excessive sugar intake can lead to diabetes, and 83.9% understood the relationship between diabetes and insulin irregularities. Interestingly, while 51.6% of participants believed diabetes is curable, 48.4% disagreed. Additionally, all participants correctly identified a fasting blood sugar level of 200 mg/dl as high. Notably, 87.1% of participants prioritized diet and exercise over medication for controlling diabetes. Financial Impact and Healthcare Access Financial burden remains a significant concern for many diabetic patients. While 64.5% of participants reported no difficulty affording their medication, a smaller group (6.5%) found it extremely difficult. Furthermore, only 16.1% had skipped or reduced their medication due to cost. Access to healthcare services was also a crucial factor, with 58.1% of patients visiting their doctor every 4-6 months, and 71% living within 5 km of their healthcare provider. The majority used private vehicles (67.7%) to visit healthcare providers, followed by public transport (29.0%). Figure 2: Bar Chart of the Study Population Based on the Effectiveness of Treatment on Percentage Reduction
Clinical Profile and Patterns of Headache in Patients Attending a Tertiary Care Hospital
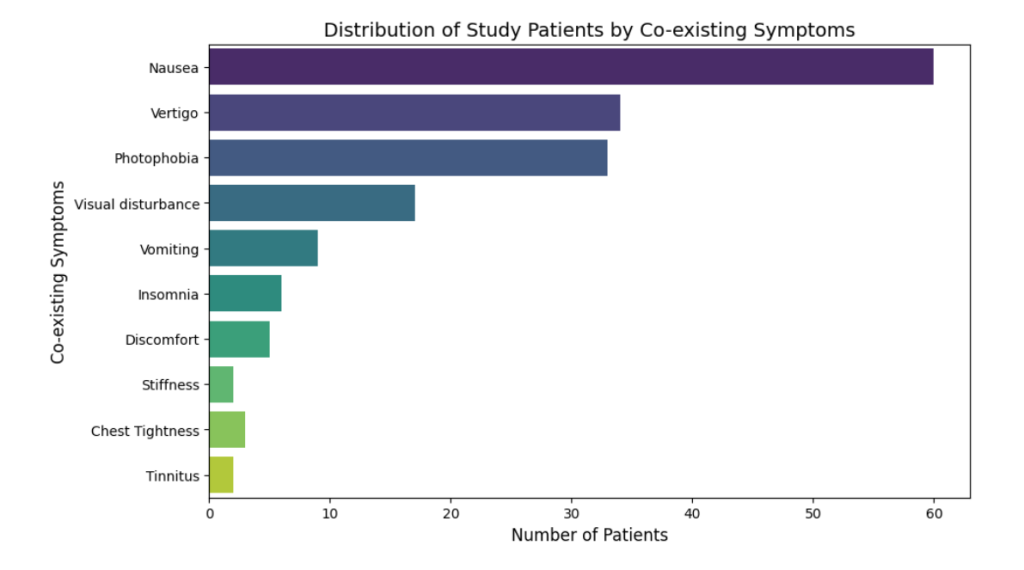
A hospital-based observational study conducted by the Neurology Department at Dhaka Medical College Hospital (DMCH) from July to December 2013 aimed to explore the characteristics and patterns of headaches in 100 patients. The study found that headaches were most prevalent among younger individuals, with 50% of patients aged between 21 and 30 years, and a notable gender disparity, as 75% of the patients were female. Housewives represented the largest occupational group, comprising 57% of the participants. In terms of headache duration, the majority of patients (64%) experienced headaches lasting between 1-6 hours, while 63% reported continuous headaches. Other significant patterns included a variety of headache characteristics, with 61% describing their headaches as compressive, and 33% reporting a pulsatile sensation. Additionally, the study revealed that many patients experienced co-existing symptoms, with nausea being the most common, affecting 60% of participants, followed by vertigo (34%) and photophobia (33%). Other symptoms such as visual disturbances, vomiting, and insomnia were also prevalent. This study highlights the high burden of headaches in younger women and housewives, providing valuable insights into the duration, frequency, and associated symptoms, which can assist healthcare providers in improving the management and treatment of headache sufferers.
Short-term Outcome of Pharmaco-Invasive Strategy (PIs) in Comparison with Delayed Primary PCI: A Single Centre Study
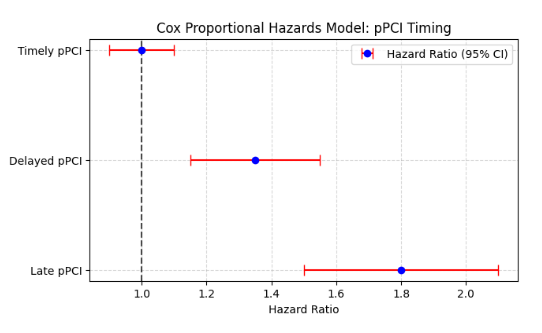
Figure 1: Cox Proportional Hazards Analysis of pPCI Timing and Survival Risk Primary percutaneous coronary intervention (pPCI) remains the gold standard for treating ST-elevation myocardial infarction (STEMI), yet disparities in treatment timelines, clinical profiles, and outcomes persist between patient groups. A comparative analysis between Group I (n=59) and Group II (n=45) revealed a predominance of male participants in both cohorts, with 84.74% in Group I and 93.33% in Group II. Despite a non-significant difference in sex distribution (p=0.896), significant variations emerged in cardiovascular risk factors. Hypertension (HTN), diabetes mellitus (DM), dyslipidemia (DL), and chronic kidney disease (CKD) were notably higher in Group I, with smoking history and family history of coronary artery disease (CAD) also significantly greater (p=0.003). Clinically, anterior STEMI was more frequent in Group I (50.84% vs. 8.98%), whereas inferior STEMI was more evenly distributed (49.15% vs. 37.28%). Although cardiogenic shock rates were higher in Group I (32.20% vs. 20.33%), this difference was not statistically significant (p=0.60). Killip classification assessments showed comparable distributions across severity classes. Treatment modalities varied considerably, with Group I utilizing low molecular weight heparin (LMWH) at a higher rate (74.57% vs. 0%), while Group II relied more on streptokinase (55.56% vs. 10.16%), though these differences lacked statistical significance. A major discrepancy in the time interval from symptom onset to first medical contact (FMC) was observed, with only 2.22% of Group II patients presenting within three hours compared to 35.59% in Group I, highlighting delayed care-seeking behavior (p=0.002). Total ischemic time comparisons showed a mixed pattern, with no significant disparities. Angiographic findings identified single-vessel disease (SVD) as predominant in both groups, though multi-vessel involvement differed slightly. The left anterior descending (LAD) artery was the primary culprit in 61.01% of Group I and 33.89% of Group II, with no statistical significance. Figure 2: Survival Curves for Different pPCI Strategies Over Time TIMI flow post-procedure, a critical determinant of reperfusion success, revealed a stark contrast, with 76.27% of Group I achieving TIMI III flow compared to only 48.89% in Group II (p=0.02), underscoring superior post-procedural outcomes in Group I. Post-procedural complications such as bleeding were significantly higher in Group II (28.89% vs. 10.16%, p=0.04), while rates of cardiogenic shock, ventricular fibrillation, and mortality remained comparable. At the three-month follow-up, adverse outcomes like recurrent myocardial infarction, heart failure, and mortality showed marginal differences, reinforcing the importance of early intervention. Further stratification of Group I based on FMC-to-balloon time demonstrated a direct correlation between delayed pPCI and increased complications, with cardiogenic shock and mortality rates escalating from 16.67% to 30.00% and 5.56% to 25.00%, respectively, as treatment delays extended beyond 180 minutes. Hazard ratio (HR) analysis further confirmed that early pPCI conferred the best survival outcomes, with the lowest HR for death (1.3, adjusted HR 1.1) compared to delayed and late pPCI groups. These findings emphasize the urgent need for optimized STEMI management, reducing pre-hospital delays, and ensuring timely pPCI to improve survival and minimize post-procedural complications.
Knowledge and Attitude Regarding Cervical Cancer and Screening among the nursing Students.
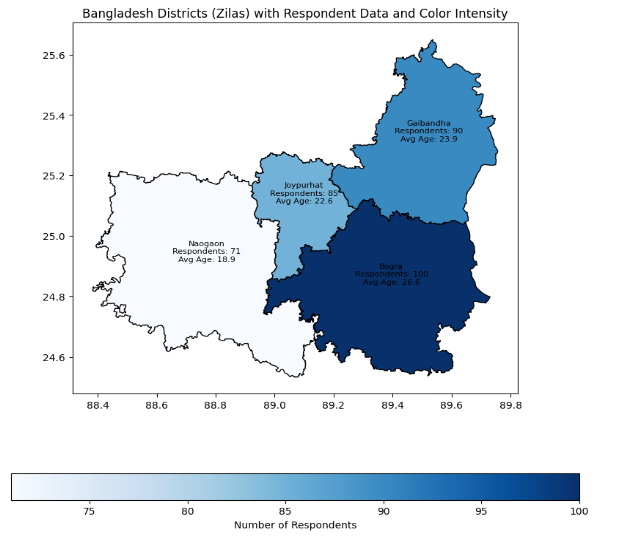
Figure 1: Respondent Distribution and Mean Age of First Delivery Across Selected Districts in Bangladesh While 77.1% had heard of cervical cancer, only 47.9% had undergone screening, with key barriers including lack of awareness (13.3%), cost (18.6%), and fear of diagnosis (10.6%). Most respondents (79.8%) believed cervical cancer is treatable if detected early, yet 9.6% were unsure about screening frequency. Although 82.4% were willing to consult a provider, 55.9% felt the health system was ill-equipped, citing inadequate personnel (69.0%) and equipment (59.5%). Additionally, 60% of those unable to access treatment were diagnosed at a late stage. Traditional and spiritual healing were still sought by 19.3% of respondents. Encouragingly, 89.1% agreed that screening is essential for all eligible women. Expanding screening programs and strengthening healthcare systems can significantly improve early detection and treatment outcomes.
Common Pattern of Congenital Heart Disease with Outcome in Sick Term and Preterm Neonates Admitted in NICU in Dhaka, Bangladesh
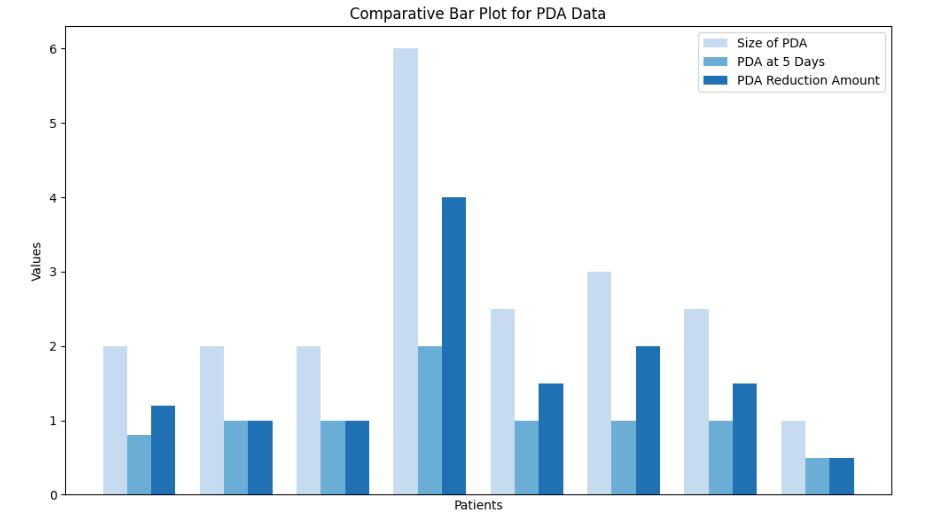
Figure I: Comparative Bar plot for PDA Data across Patients over 5 days The study “Common Pattern of Congenital Heart Disease with Outcome in Sick Term and Preterm Neonates Admitted in NICU in Dhaka, Bangladesh” explores the prevalence, clinical complications, and treatment approaches for congenital heart disease (CHD) in neonates. Among 61 cases, atrial septal defect (ASD) was the most common (36.1%), followed by ventricular septal defect (VSD) (24.6%) and patent ductus arteriosus (PDA) (19.7%). Respiratory distress (62.3%) and pneumonia (34.4%) were frequent complications, with oxygen therapy (68.9%) being the primary treatment. The study highlights the significant burden of CHD, especially in infants of diabetic mothers, and emphasizes the importance of early diagnosis and echocardiographic monitoring to improve neonatal outcomes. Figure 2: Distribution of PDA Status at 3-Month Follow-Up
Evaluating the Success of Current Standard of Care in Breast Cancer Treatment: A Retrospective Study in Bangladesh
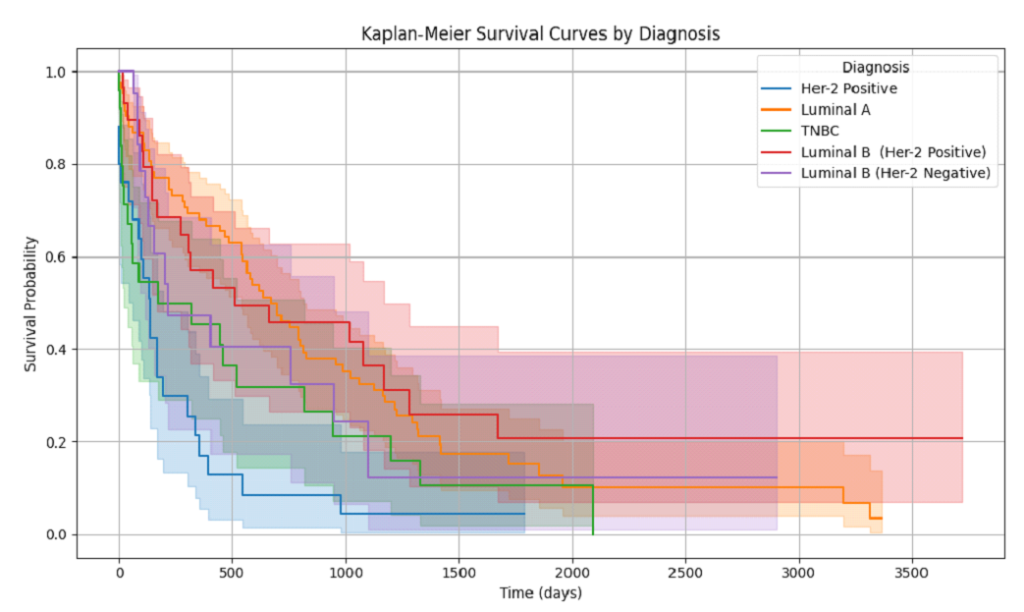
Figure: Kaplan-Meier Survival Curves by Diagnosis Group with Survival Probabilities at 30, 90, 180 and 365 Days. Breast cancer is the most common cancer among women worldwide and poses a significant public health problem, especially in low-income countries and low- and middle-income countries (LMICs) such as Bangladesh, where late diagnosis, limited resources, and inadequate treatment are common. According to GLOBOCAN, breast cancer accounts for 25% of new cancer cases in women worldwide, with an estimated 2.3 million cases and 685 thousand deaths reported in 2020. While high-income countries benefit from advanced diagnostic and therapeutic technologies, low- and middle-income countries face challenges such as limited knowledge, community culture, and limited oncology resources, leading to poor outcomes. Due to the high incidence of breast cancer in Bangladesh, the most common treatment modality is mastectomy, while the use of breast implants is limited. This study evaluated the efficacy of standard treatment in Bangladesh in terms of progression-free survival (PFS), overall survival (OS), and specific outcomes. Luminal A subtypes showed the most favorable prognosis, while triple negative breast cancer (TNBC) and HER2 positive subtypes exhibited the most severe disease and poor outcomes. Kaplan-Meier analysis showed a significantly reduced chance of survival in the first year, highlighting the urgent need for improvements in early detection and treatment. Closing this gap will require strengthening national health systems, developing advocacy plans, and investing in research and development to improve care and reduce costs. This study highlights the urgent need for interventions within limited resources to address inequalities in cancer management and improve patient outcomes.